
Charlotte, North Carolina is facing a boarding crisis in its emergency rooms, with limited and inefficient mental health care in ERs leading to shortages of psychiatric beds. This represents some of the effects of the dual diagnosis gap that exists in Charlotte, North Carolina and areas across our state.
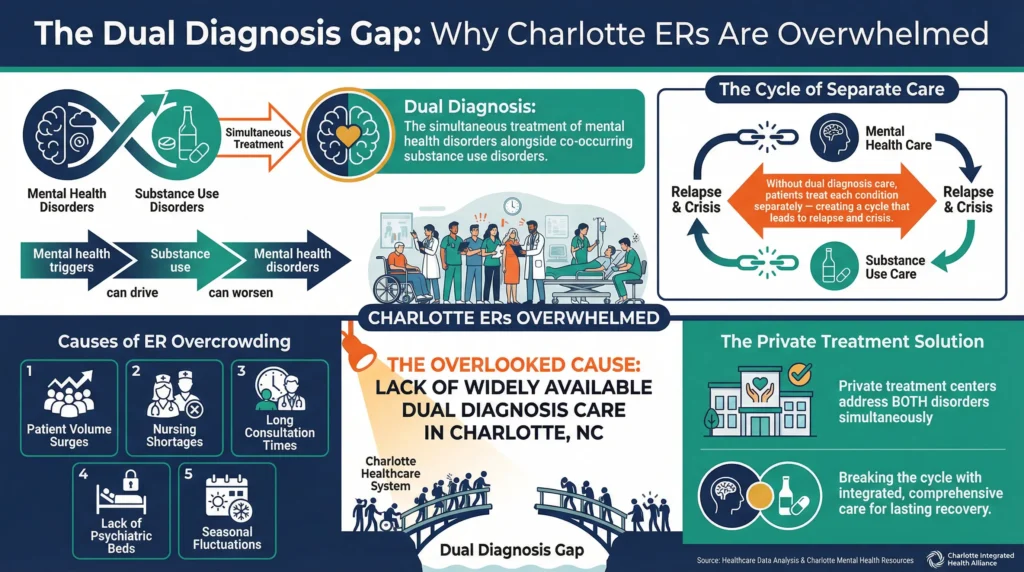
Dual diagnosis refers to the simultaneous treatment of mental health disorders alongside any co-occurring substance use disorders. Dual diagnosis care is necessary because mental health triggers can contribute to an individual’s substance use disorder, and vice versa. Due to this, some individuals have to have both disorders addressed simultaneously in order to untangle the connection and properly address the underlying relationship between the two.
At Southeastern Recovery Center, we’re sounding the alarm on how the mental health crisis in North Carolina as emergency rooms are overcrowded showcases the need for private treatment centers to provide dual diagnosis care like ours. Otherwise, we may continue seeing an impeded healthcare system that results in improper care for all North Carolinians.
Article TL;DR: Charlotte emergency rooms are increasingly overcrowded due to severe mental health events. Expansion of dual diagnosis care would help individuals get the help they need before they wind up in the emergency department.
Article Preview:
Overcrowding in Charlotte’s Emergency Rooms. Charlotte has had a developing issue where North Carolinians are having to wait for access to hospital beds and psychiatric beds due to overcrowding in emergency rooms.
The Impact Of Overcrowding In Emergency Rooms. Overcrowding in emergency departments results in worse outcomes, including premature discharges, misdiagnosis, and staff reduction in hospitals.
Why Are Charlotte Emergency Departments Overcrowded? While overcrowding in general can be the result of long consultation times and seasonal fluctuations, a lack of widely available dual diagnosis care in Charlotte likely contributes to overcrowding as well.
Why Emergency Room Mental Health Care Falls Short Of Private Treatment Like Southeastern Recovery Center. Emergency room mental health care is meant to be quickly implemented in the case of life-threatening events, which means it isn’t as effective at tackling long-term impact as private treatment facilities like Southeastern Recovery Center
FAQs about The Dual-Diagnosis Gap: Why Charlotte ERs are Overcrowded. Learn answers to frequently asked questions about dual diagnosis and the impact on overcrowding in Charlotte’s emergency rooms.
Overcrowding in Charlotte’s Emergency Rooms
The overcrowding in Charlotte, North Carolina’s emergency rooms has been an ongoing issue for years now. North Carolinians that find themselves in the midst of a mental health crisis often need immediate assistance, which leads to them going to emergency rooms. The problem is that getting a psychiatric hospital bed has increasingly become an issue.
According to a report from Charlotte’s very own WFAE, an average of 350 North Carolinians each day in January waited in emergency rooms even after they needed a hospital bed. This is because there were no psychiatric beds available, whether they were looking in the state hospital, or a nonprofit or for-profit hospital (Atrium or Novant).
Unfortunately, this isn’t a new phenomenon in North Carolina’s medical systems. Back in 2022, emergency department data from hospitals showed an elevated rate of patient visits, including pediatric patient visits. This came from young people experiencing mental health disorders such as depression, which was largely attributed to knock-on effects from the COVID pandemic.
UNC Medical Center’s main psychiatric clinic saw a 150 percent increase in patients per month from spring 2020 to spring of 2022. Additionally, involuntary commitment petitions increased by at least 97 percent from 2011 to 2021.
At the time that report, North Carolina was ranked as the 44th state nationally when it came to access to mental health care.
What we’re seeing is an ongoing problem that has only continued to grow more severe over the past few years. Charlotte’s emergency rooms are overcrowded, and this is persisting despite initiatives and efforts to increase North Carolinians’ access to mental health care services.
Charlotte and Mecklenburg County Mental Health Crisis: Key Statistics (2023 to 2026)
Charlotte and Mecklenburg County are at the center of a statewide mental health and psychiatric bed crisis that has been building for years. The statistics below reflect the current scope of that crisis, from daily ER wait times to overdose deaths in our own backyard.
| Metric | Finding |
|---|---|
| NC adults with a behavioral health disorder | 1 in 5 adults [1] |
| NC adults with serious mental illness | 1 in 18 adults [1] |
| NC adults with a substance use disorder | 1 in 6 adults [2] |
| NC youth ages 12 to 17 with a substance use disorder | 1 in 13 youth [2] |
| Share of NC mental health needs currently being met | Only 13% [1] |
| NC national ranking for behavioral health care access | 50th out of 50 states [1] |
| NC patients waiting in ERs daily for a psychiatric bed | Approximately 350 per day [3] |
| Median time a psychiatric patient spends in a Charlotte-area ER before leaving without treatment | 5.25 hours [1] |
| Average ER length of stay for an admitted psychiatric patient | 20.5 hours (1,235 minutes) [4] |
| Total NC state psychiatric hospital beds | 901 beds statewide [5] |
| Psychiatric beds sitting empty daily due to staffing shortages | Approximately 300 beds offline [5] |
| Closed patient units across NC state psychiatric hospitals | 12 of 47 units closed [6] |
| Average wait time for a psychiatric hospital admission in NC | 148 days (approximately 5 months) [5] |
| Decline in NC state psychiatric hospital admissions since 2013 | 73% decrease (3,210 to 875 admissions) [6] |
| Opioid overdose deaths in Mecklenburg County in 2023 | Nearly 300 residents [7] |
| Rise in overdose deaths among Black and Hispanic Mecklenburg County residents since 2019 | 200% increase [8] |
| NC overdose death rate in 2024 | 26.6 per 100,000 residents (2,934 total deaths) [9] |
[1] North Carolina Institute of Medicine (NCIOM), Confronting North Carolina’s Behavioral Health Crisis, 2025 [2] NC Department of Health and Human Services (NCDHHS), cited in NCIOM, 2023 [3] WFAE Charlotte, The Mental Health Crisis in North Carolina’s Emergency Rooms, 2024 [4] NC College of Emergency Physicians, Boarding Talking Points, 2023 [5] NC Health News, Who Gets a Bed in NC’s State Psychiatric Hospitals and Who Waits, February 2026 [6] Becker’s Behavioral Health, North Carolina Psych Admissions Fall 73% as 300 Beds Sit Unused, February 2026 [7] KFF Health News, Hit Hard by Opioid Crisis, Black Patients Further Hurt by Barriers to Care, 2023 [8] Mecklenburg County Public Health, Overdose Deaths Among Black and Hispanic Residents Report, 2025 [9] NC Division of Public Health, North Carolina Overdose Epidemic Data, 2024
The Impact Of Overcrowding In Emergency Rooms
- Overcrowding in emergency departments is associated with increased frequency of care discontinuation and mortality.
- Overcrowding in emergency rooms also impedes job satisfaction and can result in staff reduction in hospitals.
- Overcrowding is also associated with higher return visits, many patients have to return to emergency rooms due to premature discharges, misdiagnosis, or failure of treatment or discharge planning.
In short, overcrowding doesn’t just impact North Carolinians that are experiencing a mental health crisis and need immediate assistance. The impact is everyone going in and out of the emergency department, including the staff.

Why Are Charlotte Emergency Departments Overcrowded?
In general, overcrowding in emergency departments has several different causes including:
- Increases in the volume of patients arriving and waiting to be seen (which is sometimes directly related to the malfunctioning of healthcare services in the community)
- Emergency room nursing staff shortages
- Long consultation times
- Lack of boarding and available hospital beds
- Seasonal fluctuations
Factors related to general traffic and emergency rooms can coincide with impaired mental health and North Carolinians communities. For example, cold months and flu season can lead to higher traffic and less beds available, but this coincides with cold months correlating with higher rates of mental health disorders such as seasonal affective disorder (SAD).
Charlotte Emergency Room vs. Southeastern Recovery Center: Which Is Right for You?
Emergency rooms save lives during acute crises, but they are not built for long-term recovery. The comparison below shows where Charlotte ERs fall short for dual diagnosis patients and where private treatment at Southeastern Recovery Center fills that gap.
| Care Factor | Charlotte Emergency Room | Southeastern Recovery Center |
|---|---|---|
| Primary focus | Immediate crisis stabilization | Long-term recovery and root-cause treatment |
| Dual diagnosis treatment | Not a primary service; only 18% of addiction programs are Dual Diagnosis Capable nationally [1] | Core program offering, treating mental health and SUD simultaneously |
| Personalized treatment plans | Standardized, speed-driven protocols | Individualized plan for every patient |
| Time spent with each patient | Hours or less | Weeks to months of sustained care |
| Identifies individual triggers | No capacity for in-depth assessment | Yes, through extended evaluation and therapy |
| Evidence-based therapy (CBT, DBT) | Not offered | Central to every treatment plan |
| Detox coordination | Stabilization only | Facilitation into appropriate detox programs |
| Aftercare and sober living support | Rarely offered | Included as part of every discharge plan |
| Relapse prevention | Not offered | Core component of the program |
| Best suited for | Active, life-threatening crisis events | Sustained recovery before or after a crisis event |
| Prevents future ER visits | No | Yes, by addressing the root causes that lead to ER visits |
| Serves Charlotte and surrounding areas | Multiple Charlotte metro hospital locations | Concord, NC, serving Charlotte, Mecklenburg County, and the greater Charlotte region |
That said, there is one overlooked cause of overcrowding in Charlotte emergency rooms: the lack of widely-available dual diagnosis care.
Dual diagnosis care refers to the process of treating mental health disorders alongside substance use disorders. This is because one type of disorder may inform the other, such as an individual experiencing anxiety and turning to alcohol use the self medicate, resulting in developing an alcohol addiction.
The reason that a lack of dual diagnosis care can contribute to overcrowding and emergency departments is because individuals may be seeking treatment for their substance use disorder or the mental health disorder independently, without realizing that the two can be linked. As a result, they’ll have a hard time reaching and maintaining sobriety due to the conditions being linked to triggering each other.
The result is that individuals may be trapped in a negative loop that eventually results in them going to an emergency room because of a serious event, such as suffering from an addiction related overdose or severe withdrawal symptoms.
At Southeastern Recovery Center, we’re committed to providing dual diagnosis care to North Carolinians that are experiencing both mental health disorders and substance use disorders simultaneously we personalize all of our treatment plans in order to assure that individuals are able to find healthier coping mechanisms to reduce the odds of relapse, overdose, or ending up in the emergency room.
Why Charlotte Emergency Room Overcrowding Keeps Getting Worse: Causes and Consequences
Overcrowded emergency rooms do not just affect patients in crisis. The consequences ripple across the entire care system, from staff shortages to racial health disparities right here in Mecklenburg County. The table below outlines what happens when dual diagnosis goes untreated and ER overcrowding is left unaddressed.
| Consequence | Evidence |
|---|---|
| Higher rate of patient return visits to the ER | Overcrowding is directly linked to increased return visits within 72 hours [1] |
| Premature discharge from the ER | Boarding patients face higher rates of early, incomplete discharge [1] |
| Staff burnout and hospital workforce reduction | Overcrowding impairs job satisfaction and drives staff reduction [2] |
| NC state hospital staff vacancy rate in 2025 | 26% overall vacancy, up from 13% in 2015; includes 380 healthcare technician vacancies and 314 RN vacancies [3] |
| Relapse risk for untreated dual diagnosis patients | 2 times more likely to relapse than single-diagnosis patients [4] |
| NC patients with SUD who also have an unaddressed mental health condition | 76% carry both diagnoses at hospital discharge [5] |
| Racial health disparity in Mecklenburg County overdose deaths | 200% rise among Black and Hispanic residents vs. 14% among White residents since 2019 [6] |
| Psychiatric admissions decline despite rising demand in NC | 73% fewer admissions since 2013; patients are not being served, not recovering [3] |
| Adolescents with co-occurring major depression and SUD who received no treatment | 27.9% received zero care [7] |
[1] Kim et al., Influence of Overcrowding in the Emergency Department on Return Visit within 72 Hours, Journal of Clinical Medicine, 2020 [2] Crook et al., Workplace Factors Leading to Planned Reduction of Clinical Work among Emergency Physicians, Emergency Medicine Australasia, 2004 [3] Becker’s Behavioral Health, North Carolina Psych Admissions Fall 73% as 300 Beds Sit Unused, February 2026 [4] Tandfonline, Concurrent Disorders and Treatment Outcomes: A Meta-Analysis, 2025 [5] North Carolina Institute of Medicine (NCIOM), Confronting North Carolina’s Behavioral Health Crisis, citing 2021 NC hospital discharge data, 2025 [6] Mecklenburg County Public Health, Overdose Deaths Among Black and Hispanic Residents Report, 2025 [7] SAMHSA, 2024 National Survey on Drug Use and Health (NSDUH), 2024
Why Emergency Room Mental Health Care Falls Short Of Private Treatment Like Southeastern Recovery Center
When weighing emergency room mental health care versus private care for mental health disorders (such as what we provide at Southeastern Recovery Center), the primary factor to consider is time.
When individuals are having serious episodes relating to mental health care or substance use, a visit to the ER can save their lives. However, in the moments leading up to that serious event, and for the moments afterwards, private treatment centers like Southeastern Recovery Center can be more effective than emergency rooms.
This is because Southeastern Recovery Center is built to provide one-on-one care for a longer duration than emergency rooms. Emergency rooms are better suited for life-threatening crises, but private mental health and substance use treatment teaches individuals how to cope in the long term. This includes facilitation into detox facilities, making use of science back treatment methods such as dialectical behavioral therapy and cognitive behavioral therapy, and connecting patients with groups and sober living facilities as a form of aftercare.
Additionally, in the case of an individual needing dual diagnosis care to help avoid serious mental health crises, it takes time to identify the person’s individual triggers for both mental health disorders and substance use disorders. Private treatment facilities like Southeastern Recovery Center can afford to take time to understand each individual’s case, while emergency room psychiatric care is more focused on speed and immediate effectiveness.
While both types of treatment have their uses in North Carolina, individuals who are not experiencing an immediate, life-threatening event would be better off visiting a Charlotte treatment center like SERC rather than Charlotte’s emergency rooms.
The Dual Diagnosis Treatment Gap in Charlotte, NC: What the Numbers Show
One of the most overlooked drivers of Charlotte’s ER overcrowding is the dual diagnosis treatment gap. The data below shows just how many North Carolinians are living with both a mental health disorder and a substance use disorder, and how few are receiving care that addresses both at the same time.
| The Problem | The Number |
|---|---|
| U.S. adults with both a mental illness and a substance use disorder | 21.2 million adults [1] |
| Adults with co-occurring disorders who received no treatment of any kind | 41.2% (nearly 1 in 2) [1] |
| Adults with co-occurring disorders who received treatment for both conditions | Only 14.5% [1] |
| U.S. addiction treatment programs that are Dual Diagnosis Capable | Only 18% [2] |
| U.S. mental health programs that are Dual Diagnosis Capable | Only 9% [2] |
| NC hospital patients with a substance use disorder who also had a mental health diagnosis | 76% [3] |
| Adults with serious mental illness who also have a substance use disorder | 47.3% [1] |
| Adults with a substance use disorder who also have any mental illness | 45.8% [1] |
| Relative risk of relapse for untreated dual diagnosis patients vs. single-diagnosis patients | 2 times more likely [4] |
| NC adults who needed substance use treatment and actually received it | Only 19.3% [1] |
[1] SAMHSA, 2024 National Survey on Drug Use and Health (NSDUH), 2024 [2] McGovern et al., Dual Diagnosis Capability in Mental Health and Addiction Treatment Services, PubMed/PMC [3] North Carolina Institute of Medicine (NCIOM), Confronting North Carolina’s Behavioral Health Crisis, citing 2021 NC hospital discharge data, 2025 [4] Tandfonline, Concurrent Disorders and Treatment Outcomes: A Meta-Analysis, 2025
FAQs about The Dual-Diagnosis Gap: Why Charlotte ERs are Overcrowded
Is Charlotte experiencing overcrowding in its emergency rooms?
Yes, Charlotte, North Carolina has been experiencing an increasing amount of overcrowding in its emergency rooms since the pandemic.
How does North Carolina rank nationally when it comes to access to mental health care?
North Carolina was ranked as the 44th state nationally when it came to access to mental health care in 2022.
How does dual diagnosis care impact overcrowding and Charlotte emergency rooms?
Because dual diagnosis care is not widely available in Charlotte, individuals suffering from both substance use disorders and mental health disorders may be unable to get the proper treatment they need to avoid triggers, which can lead to them ending up in a Charlotte ER.
What are some other causes of overcrowding in emergency rooms?
Other causes of overcrowding in emergency departments include staff shortages, increased volume of patients arriving and waiting to be seen, and seasonal fluctuations.
Sources:
Crook, Heather D., et al. “Workplace Factors Leading to Planned Reduction of Clinical Work among Emergency Physicians.” Emergency Medicine Australasia : EMA, vol. 16, no. 1, Emergency medicine Australasia : EMA, 1 Feb. 2004, pp. 28–34, https://doi.org/10.1111/j.1742-6723.2004.00531.x.
Kim, Dong-uk, et al. “Influence of Overcrowding in the Emergency Department on Return Visit within 72 H.” Journal of Clinical Medicine, vol. 9, no. 5, MDPI AG, 9 May 2020, p. 1406, https://doi.org/10.3390/jcm9051406.
Knopf, Taylor. “New Mental Health Data Show ‘Unsustainable’ Burden on NC Hospitals.” North Carolina Health News, 22 Aug. 2022, https://www.northcarolinahealthnews.org/2022/08/22/emergency-department-burden-shown-in-mental-health-data/.
Menon, Nisha Vengassery Balakrishnan, et al. “Bed Utilization and Overcrowding in a High-Volume Tertiary Level Pediatric Emergency Department.” Indian Pediatrics, vol. 58, no. 8, Indian pediatrics, 15 Aug. 2021, pp. 723–725, https://pubmed.ncbi.nlm.nih.gov/33634795/.
“Part 5: The Mental Health Crisis in North Carolina’s Emergency Rooms.” WFAE 90.7 – Charlotte’s NPR News Source, https://www.wfae.org/podcast/fractured/2024-05-03/the-mental-health-crisis-in-north-carolinas-emergency-rooms.





